Worried about a lump you have noticed coming out of your vagina?
Of the hundreds (perhaps thousands) of women I have seen with prolapse, every single one of them was worried when they found it. It is very disconcerting to notice a lump in the vagina. Most of the women I see initially feared the worst. (When you find something in your vagina that wasn’t there before, you should head straight to your doctor.) But for the vast majority of women I see, it was not something life-threatening. It was a vaginal prolapse.
Aside from a vaginal lump or bulge, other symptoms of prolapse include:
- A feeling of incomplete emptying when you pee or do a poo
- A dribble when you go to stand up off the toilet
- A feeling that you need to press to help do a poo (e.g. just in front of the anus, or inside the vagina, pushing back)
- Your flow is different to before when you pee
- A dragging feeling at the vaginal opening when standing, especially for a long time
These symptoms do not mean you have a prolapse. They can be symptoms of other things, so it’s important you get an individualised assessment.
Most people think that a prolapse means that your uterus is falling out of the vagina. But a vaginal prolapse means that any one of the pelvic organs is bulging into the vagina. This could be the bladder, the uterus, or part of the bowel. So if the uterus has been removed (a hysterectomy), it is still possible to have a prolapse. This is because the bladder or bowel can prolapse, but also the vagina itself (like a sock turning inside out).
Your organs are not going to fall out onto the floor with a prolapse.
This is one key thing to understand. Damage to the support for the organs can make them drop down, but they are always still connected to you. Prolapse is more like a hernia: when an organ bulges into a space it’s not supposed to be in.
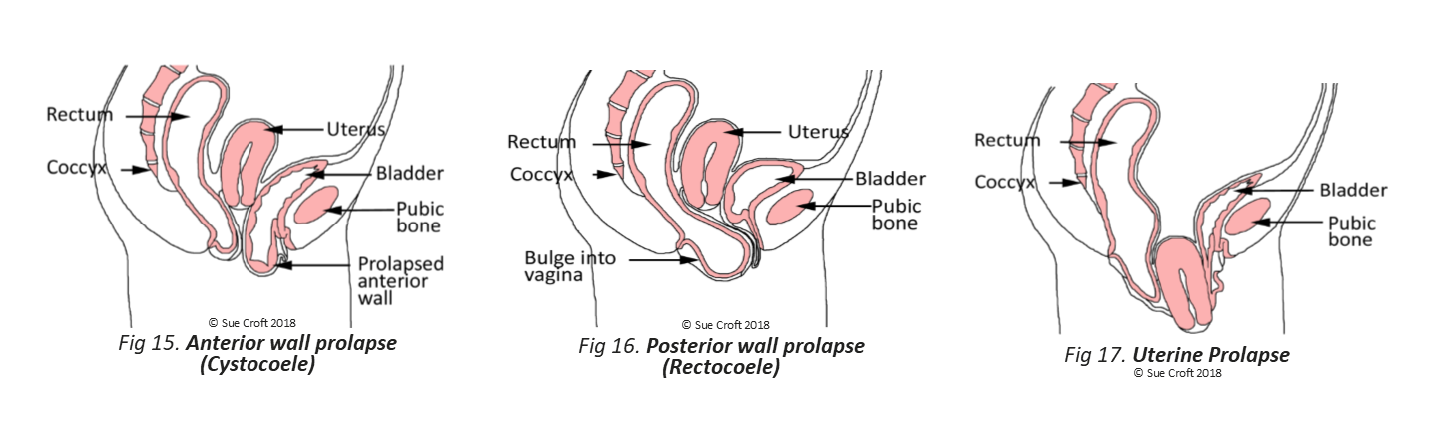
A bladder prolapse is when the bladder loses its support and bulges down and backwards into the vagina. This is called a cystocoele. If just the urethra (bladder tube) drops down, it’s called urethrocoele. When the uterus drops down the vagina, it’s called a uterine prolapse. When the rectum bulges down and forwards into the vagina, it’s called a rectocoele.
Here are some images from Sue Croft’s wonderful book: Pelvic Floor Essentials, which you can buy here!
Pictures of prolapse can be scary.
In fact, even the word “prolapse” is scary! But keep in mind some prolapses are very mild. In fact, it can be so mild that it doesn’t give you symptoms. But that’s no reason to be complacent. Prolapse can (and often does) get worse if you don’t do anything about it.
Getting your pelvic floor muscles in the best shape possible is one of the best things you can do for your prolapse. You will need to see a pelvic floor physiotherapist for this to get the right exercises for you. You also might find it helpful to read Sue Croft’s Pelvic Floor Essentials (truly essential reading for all women!) and to read my blog posts on Top Ten Pelvic Floor Mistakes, and Top Tips for Sticking With Your Pelvic Floor Exercises.
It’s important to know the do’s and don’ts, and a pelvic floor physiotherapist can help you with this.
Many women feel nervous about having sex with a prolapse.
I’ve written a separate blog post on sex and prolapse here.
The right general exercise is also critical. A pelvic floor physiotherapist will also give you individualised advice on what general exercise will be best. Certain types of exercise can make it worse. I have, sadly, often seen women where it came on after starting the wrong kind of exercise program. While it’s most common in women who have had a baby, straining to do a poo also helps bring it on. So can heavy work like gardening, renovating or moving house. Excess tummy fat also makes it worse.
At Equilibria, we use a combination of physiotherapy and nutrition to address all the major factors: pelvic floor problems, bowel and gut problems, excessive abdominal fat and poor posture and movement habits.